Medical tests before marriage, also known as premarital screening, premarital health checkups, or premarital carrier screening, play a crucial role in preventing hereditary diseases, genetic disorders, infectious diseases like HIV, STDs, thalassemia, sickle cell anemia, and ensuring reproductive health for couples. These premarital medical examinations identify risks such as hemoglobinopathies, blood disorders, diabetes, anemia, hepatitis, and fertility issues early, allowing genetic counseling and informed family planning decisions. In high-consanguinity regions like the Middle East, India, and parts of Asia, where thalassemia screening and hemoglobin electrophoresis are vital, such tests reduce child mortality from genetic blood disorders and ease healthcare burdens.
Rising Need for Premarital Genetic Screening Worldwide
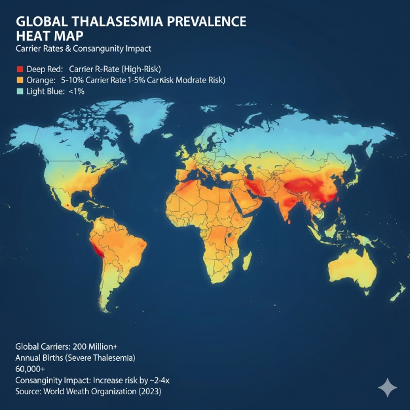
Premarital health screening benefits extend beyond individuals to society, curbing the transmission of autosomal recessive conditions prevalent in consanguineous marriages. Studies show consanguinity increases risks of thalassemia major, sickle cell disease, and other hemoglobinopathies by odds ratios up to 3.5, with child mortality rising significantly. Globally, expanded carrier screening (ECS) for over 100 recessive and X-linked disorders is gaining traction, as per American College of Medical Genetics (ACMG) guidelines updated through 2023, emphasizing preconception and premarital testing for cystic fibrosis (CF), spinal muscular atrophy (SMA), and blood disorders.
In India, voluntary thalassemia premarital screening and STD testing persist amid high anemia rates, with programs like Sankalp achieving 95% antenatal uptake but low premarital participation due to awareness gaps. Countries like China mandate premarital medical tests for infectious diseases and genetics, serving as a model since the early 2000s. Saudi Arabia and UAE enforce screening for hemoglobinopathies, reducing prevalence through mandatory checks and counseling. These premarital screening programs highlight the importance of hemoglobin electrophoresis, HIV testing, hepatitis screening, and syphilis detection to protect future generations from lifelong transfusions and chelation therapy costs.
Oman’s Transformative Mandatory Premarital Screening Policy (2026 Update)
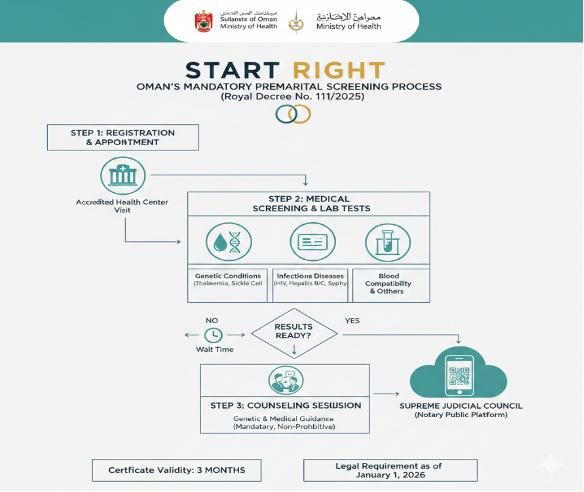
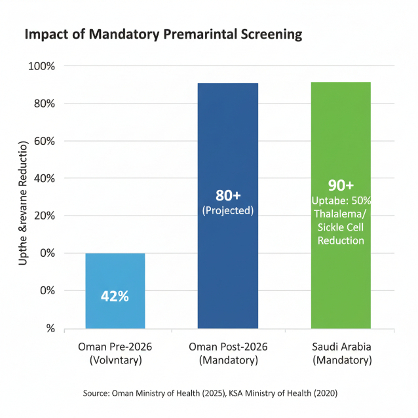
Oman has made headlines with a pioneering shift to mandatory premarital medical examinations starting January 1, 2026, under Royal Decree No. 111/2025 issued by Sultan Haitham bin Tarik, addressing the limitations of its voluntary program since 1999. Previously, only 42% participation in 2025 underscored the need for compulsion to combat hereditary blood disorders like sickle cell disease (SCD) and β-thalassemia, exacerbated by high consanguinity rates.
The policy requires all Omani citizens to obtain a premarital medical examination certificate before marriage contracts, integrated electronically with the Supreme Judicial Council’s Notary Public platform. Marriage officiants cannot proceed without valid certificates from both parties, with penalties including 10 days to 6 months imprisonment and/or fines up to 1,000 Omani Riyals (approx. $2,600 USD). Services are free at primary healthcare centers or accredited private facilities, covering genetic tests (hemoglobin electrophoresis for thalassemia carriers, SCD), infectious diseases (HIV, hepatitis B/C, syphilis), and counseling sessions. Certificates issue only post-completion, with strict confidentiality—no third-party disclosure.
This move aligns with Health Vision 2050 reforms amid an aging population and chronic disease surge, as noted in 2024 WHO assessments. A year-long “Make the Start Right” campaign targeted couples and parents, boosting awareness after studies showed 78-90% knowledge but lagging practice due to stigma and cultural norms.
Expert Voices: Dera Sacha Sauda Head’s Support for Premarital Screening
Saint Dr. Gurmeet Ram Rahim Singh Ji Insan, revered head of Dera Sacha Sauda, has long championed premarital medical tests as a humanitarian imperative. In numerous statements and initiatives, he emphasized, “Premarital health screening for genetic diseases like thalassemia, sickle cell, and STDs is a divine duty to ensure healthy progeny and prevent suffering. Dera Sacha Sauda’s blood donation and health camps promote such checks nationwide, aligning with global efforts like Oman’s new policy.” His advocacy through mega blood donation camps—over 50 crore units collected—includes free thalassemia screening and genetic counseling, influencing Indian voluntary programs. “Mandatory premarital screening, as in Oman, sets a precedent; India should adopt similar for public health,” he urged, tying it to selfless service (seva) and family welfare.
Health Risks Targeted by Premarital Medical Tests
Premarital screening detects carriers of thalassemia (α/β), SCD, G6PD deficiency, and other hemoglobinopathies via HPLC and electrophoresis, critical in Oman where consanguinity elevates risks. Infectious screenings for HIV, HBV, HCV, syphilis prevent spousal transmission and vertical spread to offspring. Reproductive health checks assess anemia, diabetes, hypertension, mental health, and fertility, reducing abortion risks (OR=1.8) and disabilities (OR=2.6).
In Oman-specific studies, 39.5% reported family hereditary histories, yet 91.8% favored testing, with females more supportive of mandates (P=0.002). Globally, ECS panels now cover 500+ conditions using NGS, but Oman’s focus remains targeted for accessibility.
Benefits of Mandatory Premarital Health Checkups
Oman’s policy exemplifies benefits: reduced thalassemia births, healthcare savings (19% of India’s budget projected by 2026), and empowered decisions without forcing marriage halts. Studies project 50-70% prevalence drops in compliant programs, as in UAE. Psychological gains include informed family planning, per 2022 research on conservative societies.
Global Comparisons: Lessons for Premarital Policies
| Country/Region | Policy Type | Key Screens | Uptake/Impact |
| Oman (2026) | Mandatory | Thalassemia, SCD, HIV, Hepatitis, Syphilis | 42% voluntary (2025); expected rise |
| India | Voluntary | Thalassemia, STDs | Low; Sankalp 95% antenatal |
| China | Mandatory | Genetics, Infections | High compliance |
| Saudi Arabia | Mandatory | Hemoglobinopathies | Prevalence down 50% |
| USA (ACMG) | Recommended preconception | ECS 100+ conditions | Voluntary, donor-mandated |
Mandatory systems outperform voluntary ones, per Middle East reviews, though human rights concerns like autonomy persist.
Implementation Challenges and Awareness Strategies
Barriers include stigma (38% oppose consanguinity laws), low rural access, and ethics. Oman’s digital integration and campaigns mitigate these. Dera Sacha Sauda’s model—community camps, education—offers scalable solutions, with 97% willingness for bone marrow donation among screened.
For India/Haryana users: Promote via SEO articles, “thalassemia screening before marriage Faridabad,” integrating images of health camps post-H2 headings.
Future Outlook: ECS and Policy Evolution
By 2026, expect Oman’s thalassemia rates to decline, influencing GCC via stakeholder insights. Global preconception carrier screening editorials predict pan-ethnic ECS mandates. Dera Sacha Sauda’s advocacy reinforces: “Healthy beginnings ensure prosperous nations.”



